The Heart Attack Used to Be a Death Notice. Medicine Rewrote That Story.
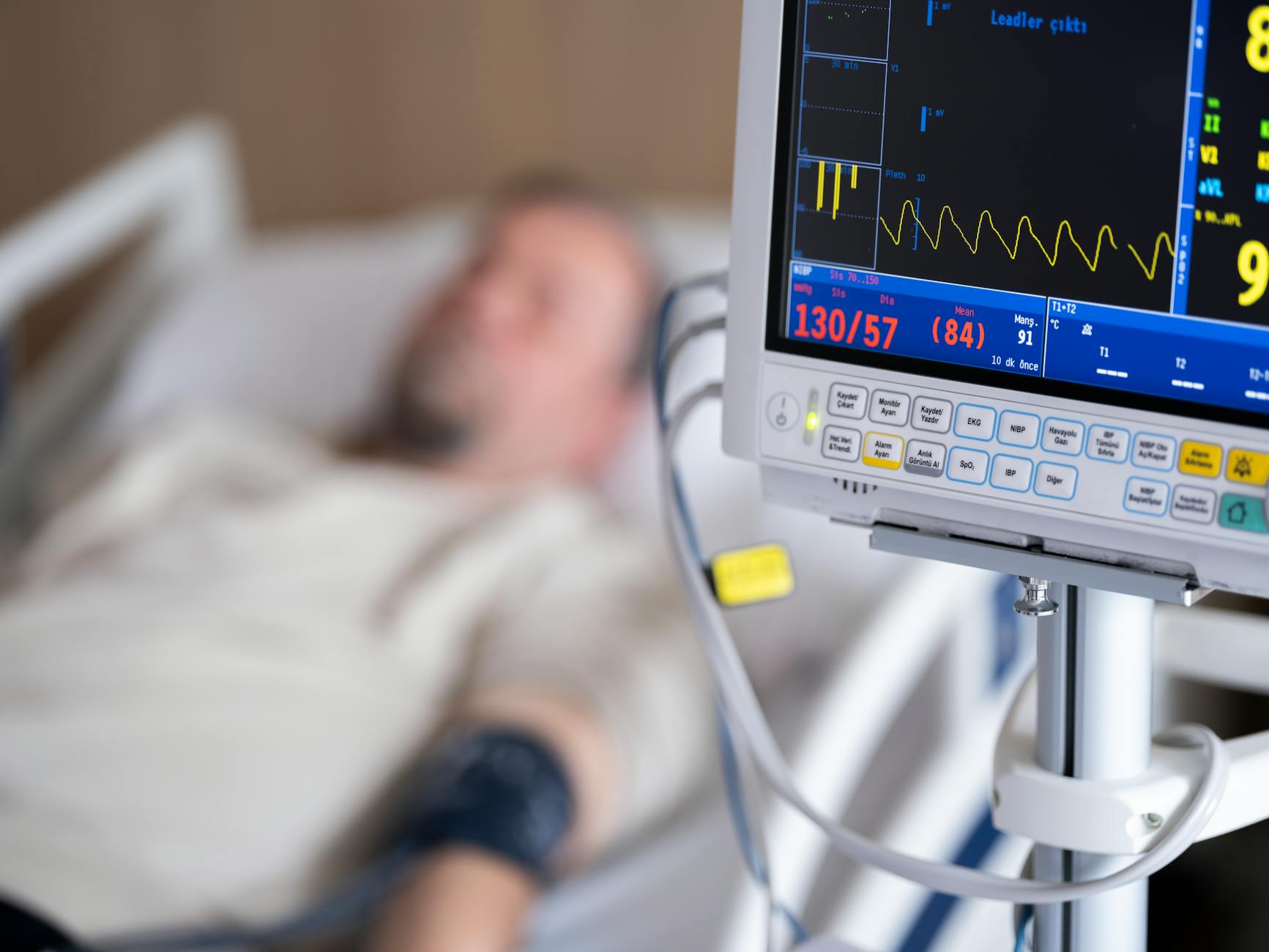
The Heart Attack Used to Be a Death Notice. Medicine Rewrote That Story.
In 1950, if you clutched your chest in pain and collapsed, the odds were not in your favor. Heart disease was already the leading cause of death in America, and a full-blown myocardial infarction — a heart attack — carried a mortality rate of somewhere between 30 and 40 percent in the hospital alone. Many more patients died in the days and weeks that followed, as damaged heart muscle weakened and failed. Surviving wasn't exactly rare, but it wasn't something you could count on, either.
Today, that in-hospital death rate has fallen to somewhere around 5 to 10 percent for patients who reach emergency care quickly. For those treated at high-volume cardiac centers with modern intervention capabilities, outcomes are even better. The same event that was a near-certain death sentence for previous generations has become a condition that millions of Americans survive and recover from every year.
That turnaround didn't happen by accident. It happened because of a series of medical breakthroughs — some dramatic, some quiet — that together rewrote what a heart attack means.
What Doctors Did in 1950 (And Why It Wasn't Enough)
To appreciate how far things have come, it helps to understand what medicine actually looked like in the mid-20th century when it came to cardiac care.
In 1950, there was no such thing as a coronary care unit. There were no defibrillators in hospitals. Doctors didn't yet have a clear picture of what was actually happening inside the arteries during a heart attack — the understanding that most attacks were caused by a blood clot blocking a coronary artery was only beginning to solidify in the medical literature.
Treatment, such as it was, consisted primarily of strict bed rest — sometimes for six weeks or more — combined with morphine for pain, oxygen, and careful monitoring. The logic was essentially: the heart has been damaged, so rest it completely and hope it heals. Patients were told not to walk, not to climb stairs, not to exert themselves in any way. Some hospitals put patients in darkened rooms to minimize stimulation.
This wasn't negligence — it was the best available medicine given what was known at the time. But it was largely passive. There was no way to open a blocked artery, no way to restore blood flow to dying heart muscle, no way to electrically restart a heart that had gone into a fatal rhythm. If the heart gave out, it gave out.
The Breakthroughs That Changed the Odds
The transformation of cardiac care happened in waves, with each decade bringing tools and techniques that would have seemed like science fiction to the generation before.
The defibrillator arrived in clinical use in the 1950s and 1960s, and its impact was immediate. Ventricular fibrillation — the chaotic, uncoordinated electrical activity that causes the heart to stop pumping effectively — had previously been a death sentence. The ability to deliver a controlled electrical shock and restore normal rhythm saved lives that nothing else could have saved. The coronary care unit, which became standard in American hospitals through the 1960s, paired continuous cardiac monitoring with defibrillation capability and immediately cut in-hospital death rates.
Clot-busting drugs, known as thrombolytics, represented the next leap. By the 1980s, clinical trials had confirmed that drugs like streptokinase and later tPA could dissolve the blood clots causing most heart attacks, restoring blood flow to the heart muscle if given quickly enough. For the first time, doctors weren't just managing the aftermath of a heart attack — they were actively intervening in the event itself. Time became the critical variable: the faster the drug was given, the more heart muscle could be saved.
Coronary angioplasty and stenting took that logic even further. First performed by Swiss cardiologist Andreas Grüntzig in 1977, angioplasty involves threading a thin catheter through the arteries to the site of a blockage, inflating a small balloon to open the artery, and — once stents became available in the late 1980s — leaving a small metal scaffold in place to keep it open. This procedure, now called percutaneous coronary intervention or PCI, became the gold standard for treating heart attacks. It's faster, more precise, and more effective than drug therapy alone.
Walk into a major American hospital today and the cardiac catheterization lab — the cath lab — is one of the most consequential rooms in the building. Patients arrive by ambulance, get wheeled directly in, and can have a blocked artery opened within 90 minutes of arriving at the door. That 90-minute benchmark, known as "door-to-balloon time," is now a national quality standard.
The Drugs That Keep Working After You Leave
The revolution in acute care — what happens in the first hours of a heart attack — gets most of the attention. But equally important is what happens after a patient goes home.
The development of aspirin therapy, beta-blockers, ACE inhibitors, and statins over the past five decades has transformed long-term survival after a heart attack. These medications reduce the risk of a second event, protect the damaged heart from further stress, and lower the cholesterol levels that contribute to arterial blockages in the first place. A patient discharged from a hospital today leaves with a pharmaceutical toolkit that simply didn't exist a generation ago.
Statins alone — cholesterol-lowering drugs that became widely prescribed from the 1990s onward — are estimated to prevent tens of thousands of cardiovascular deaths in the United States every year.
The Numbers Tell the Story
The statistics are worth stating plainly, because they're extraordinary.
In 1960, the age-adjusted death rate from cardiovascular disease in the United States was approximately 507 per 100,000 people. By 2020, that number had fallen to around 161 per 100,000 — a decline of nearly 70 percent over six decades, even as the population aged and grew. The American Heart Association estimates that roughly 18 million deaths have been prevented since 1970 due to improvements in cardiovascular treatment and risk factor management.
That's not a rounding error. That's a transformation.
Progress With Eyes Open
Heart disease remains the leading cause of death in the United States. Despite every advance, it kills roughly 700,000 Americans every year. Access to high-quality cardiac care is not equally distributed — outcomes vary significantly by race, income, and geography in ways that reflect broader inequities in the American healthcare system. And the underlying risk factors — poor diet, physical inactivity, smoking, uncontrolled blood pressure — remain stubbornly common.
The story of cardiac medicine over the past 75 years is genuinely one of the great achievements of modern science. But it's also a reminder that medical breakthroughs and population health aren't the same thing. The tools exist to save far more lives than they currently do.
What changed between 1950 and today is the medicine. What still needs to change is everything around it.